![]() With this new case of cicatricial upper eyelid ectropion I was guided by Dr. Roy W. Pelton (“Dr. Pelton” in rest of the post), through a wonderful tele-consultation system of Orbis (Cybersight Consult). Dr. Roy Pelton is a consultant oculoplastic surgeon from Colorado, USA, and thus he helped me a lot with quite a few cases.
With this new case of cicatricial upper eyelid ectropion I was guided by Dr. Roy W. Pelton (“Dr. Pelton” in rest of the post), through a wonderful tele-consultation system of Orbis (Cybersight Consult). Dr. Roy Pelton is a consultant oculoplastic surgeon from Colorado, USA, and thus he helped me a lot with quite a few cases.
So I feel it will be interesting to see the story how it was, in a chronological order, through our communication.
Jun 16 (Day 2 after burn)
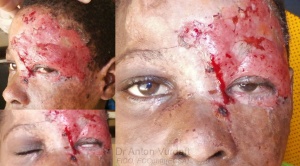
Me: This is a 8yo boy epileptic dropped himself in the fire. Got facial burns, involving both left eyelids and eyebrow. Presented 2 days ago and some amount of lagophthalmos is present already, with good Bell’s though. I am planning to apply the same treatment as in previous case, but add temporary tarsorrhaphy in hope to slow down or minimize the ectropion formation or corneal exposure at least.
Tentative plan: Tetracycline ointment tds on burnt areas. Steroid skin cream on burnt areas. Tab. Prednisolone 2 mg/kg for 10 days, than taper. Tab. Cloxacilling 250 tds for 7 days. Temporary complete tarsorrhaphy with 4-0 silk and bolsters for 3-4 weeks.
Dr. Pelton: Your plan sounds like a good one. Keep me posted on how he is doing.
Jul 14 (Day 32 after burn)
Me: Greetings, Dr. Pelton! It’s been one month now, and both eyelids ectropion starts forming. I had to redo tarsorrhaphy to prevent more exposure (SPKs++). What is the optimal timing for skin grafting in this condition? How many months should I wait? Thanks
Dr. Pelton: A few things to consider: 1. As long as there is inflammation, the grafting with be more difficult. But there are times when you just can’t wait. This may be the case. 2. I am surprised that the right lid has ectropion as well since the burns seem minimal there. 3. Can you inject the lids with Kenalog steroid to slow the inflammation? 4. where will you get skin to graft? 5. You may need to keep the lids shut for an extended length of time. Can you do a pillar tarsorraphy (conj)? Can you send recent pictures?
Me: Dr. Pelton, I meant both upper and lower lids of left eye. I have redone tarsorrhaphy (members of community wanted to be sure we haven’t removed the eye and released sutures to make sure..). So I will do next photos after 2-3 weeks I guess, when they’ll cut through, if they will. However I have triamcinolone and I can inject, thanks for advice. I guess I will need two grafts – one for upper lid from retroauricular sulcus, other for lower lid (perhaps – from the contralateral retroauricular?). Does it make sense? I will update you with pics soon. Thanks
Jul 21 (Day 39 after burn)
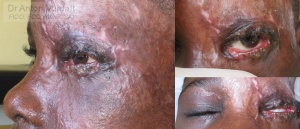
Me: Dear Dr. Pelton. Here are the new photos. Unfortunately, the second tarsorrhaphy does not work, and probably pillar tarsorrhaphy could be the better solution indeed. But anyway. Do you think this is the time for pillar tarsorrhaphy or for skin grafting? I expect a lot of scarring to continue… I can only do the injection of triamcinolone under the anesthesia, the boy had a negative experience and won’t allow doing anything while awake.
Dr. Pelton: thus far the globe looks pretty good. I might just have him lubricate aggressively for as long as possible. If you can wait 6 months from the time of injury, I think the chances of him keeping the graft are best. if the eye starts to turn red and the cornea starts to look bad, then your hand will be forced. Steroids into the wound should really help if you can ever do it (if he’s in the OR for any other reason). Topical hydrocortisone cream may help as well. Keep me posted.
Me: Thanks, will see how it goes. We started hydrocortisone cream two weeks back.
Aug 8 (Day 57 after burn)
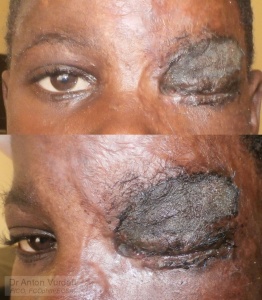
Me: Hello, Dr. Pelton. They came again with worsening. Exposure of lacrymal gland and tarsus +++, spk ++. Do you think this should be a surgery now? If yes – should it be simultaneous grafts for both upper and lower lids? Would upper arm skin suffice? Regards, Anton
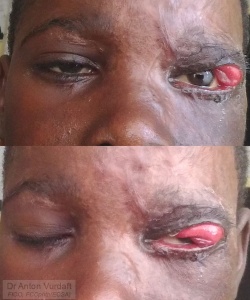
Cicatricial ectropia, both eyelids, prolapsed upper tarsus, conjunctiva and lacrimal gland, severe lagophthalmos and corneal exposure.
Dr. Pelton: I agree that you are probably now forced to do something. I think I’d just start with a large graft to the upper eyelid and see how he does with that (see pic). If the lids close well then that might be enough. If not, he might need the lower lid grafted as well. I’d consider a temporary tarsorraphy and patch for three days at least.
Aug 11 (Day 60 after burn)
Me: Dear Dr. Pelton, I will proceed to grafting of the upper lid as advised, next week. Do you think retroauricular skin can be enough again? Or should it be the upper arm skin this time? I will also do tarsorrhaphy, thanks.
Dr. Pelton: I think you’ll need to take a large graft and the upper arm will probably be the best site to obtain that.
Me: Do you think that in this case the graft should be grossly oversized due to imminent postoperative contracture?
Dr. Pelton: I would oversize it by about 1/3. Hopefully, you’ll have the luxury of removing some of it later if there is excess. You definitely would rather have too big rather than too little.
Me: Thanks, I will do my best and post the results later on.
Aug 25 (Day 74 after burn, day 7 after upper lid skin grafting)
Me: Hello, Dr. Pelton. Here is the boy after skin graft (from upper inner arm). One week post-op, sutures removed, tarsorrhaphy in situ. Graft seems taken well, and I will have them for review in 3 weeks. Thanks for guidance.
P.S. Dr. Pelton did not mind this correspondence to be published.
Continued in Part II (outcomes 2 months after surgery).