![]() Part I was here. It was the case of a young boy, who dropped himself into fire during epilepsy attack and got extensive left upper face burn with eventual upper and lower eyelids cicatricial ectropion. In Part I I described the first 74 days after he got burns, together with the repair of the ectropion of upper lid (performed in August 2017).
Part I was here. It was the case of a young boy, who dropped himself into fire during epilepsy attack and got extensive left upper face burn with eventual upper and lower eyelids cicatricial ectropion. In Part I I described the first 74 days after he got burns, together with the repair of the ectropion of upper lid (performed in August 2017).
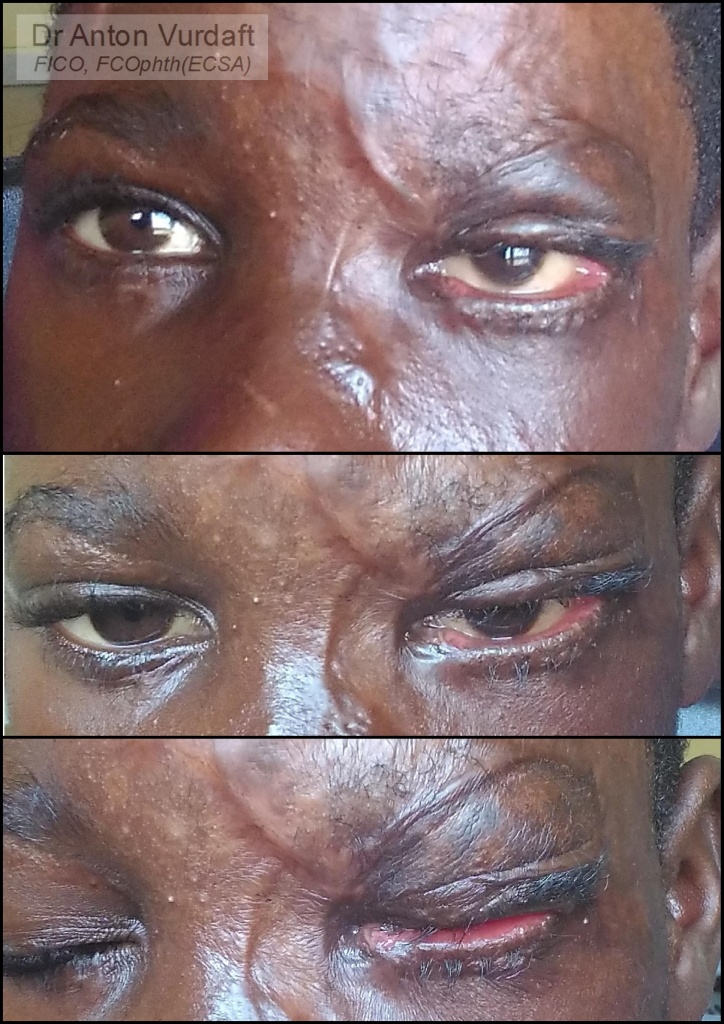
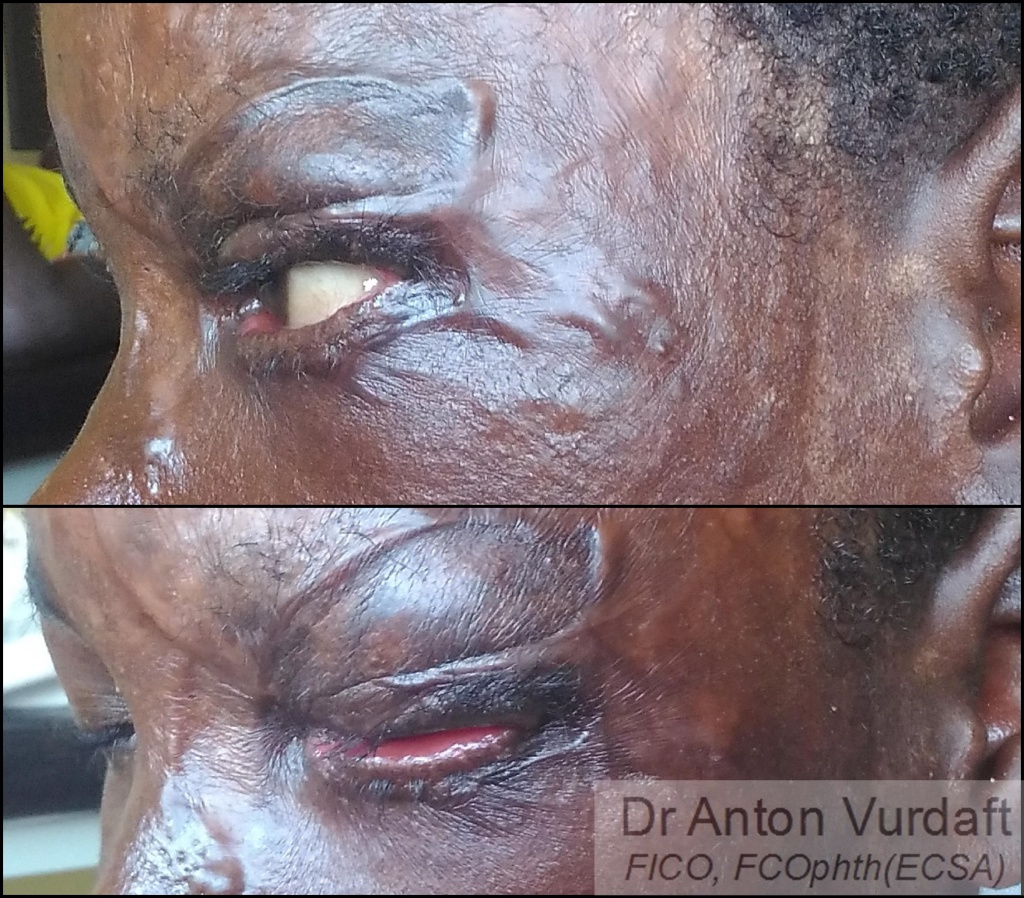
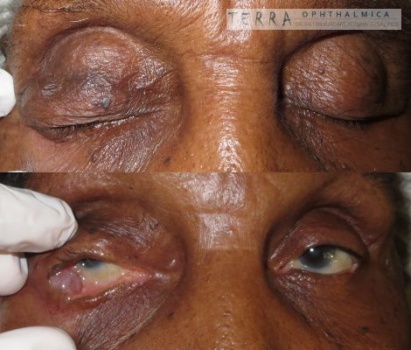
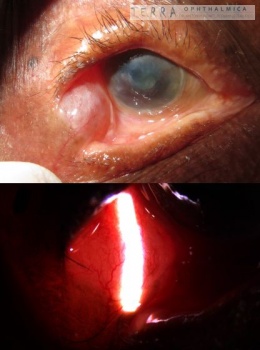
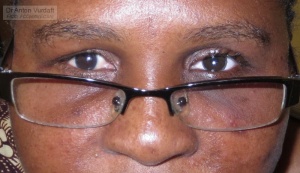
Here I will display the photos of outcome, which were taken precisely 2 months after the skin grafting for upper lid.
Lower lid cicatricial ectropion was progressing and required a surgery later. But it was definitely not that dangerous for the cornea, and the timing allowed to postpone the surgery until burn scarring process completion. I felt therefore my duty to prevent the unnecessary blindness in this kid was fully accomplished. (Lower lid surgery was performed by general plastic surgeon upon my departure from Zambia).
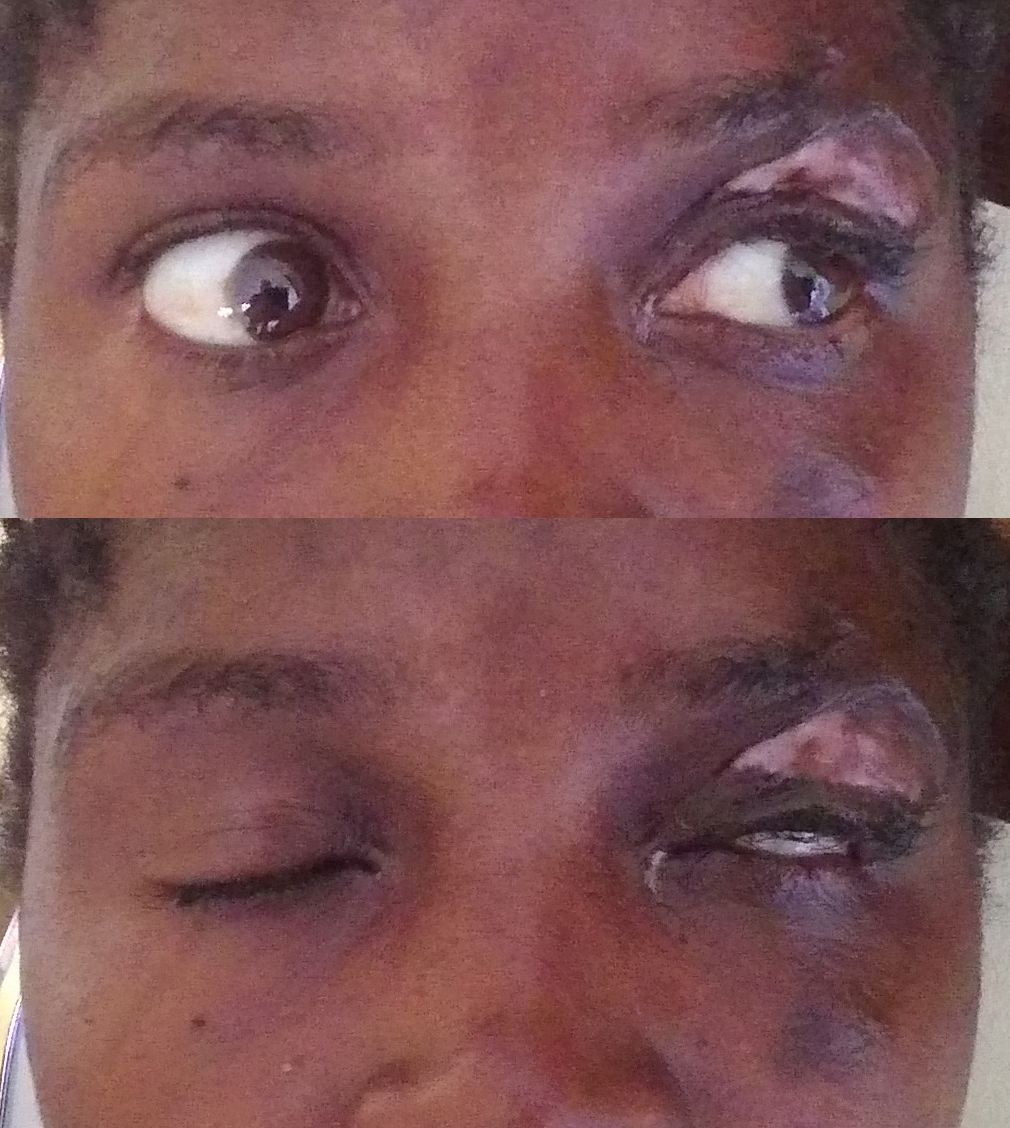
![]() Случай августа 2017 года. Хотел поделиться случаем рубцового выворота с коррекцией кожным трансплантатом (с внутренней стороны плеча) у мальчика лет 8, который пострадал в результате падения на огонь во время приступа эпилепсии. В первой части я показал прогрессирование рубцевания за первые 70 дней, что в верхнем веке было настолько выражено, что привело даже к экспозиции слёзной железы (и, естественно, роговицы). Что было неотложным показанием к операции, в других условиях проводящейся в гораздо более поздние сроки из-за прогрессирующего послеожогового рубцевания. На втором коллаже представлены фотографии 2 месяца спустя после операции рубцового выворота. Рубцовый выворот нижнего века также прогрессировал, но срочности не представлял.
Случай августа 2017 года. Хотел поделиться случаем рубцового выворота с коррекцией кожным трансплантатом (с внутренней стороны плеча) у мальчика лет 8, который пострадал в результате падения на огонь во время приступа эпилепсии. В первой части я показал прогрессирование рубцевания за первые 70 дней, что в верхнем веке было настолько выражено, что привело даже к экспозиции слёзной железы (и, естественно, роговицы). Что было неотложным показанием к операции, в других условиях проводящейся в гораздо более поздние сроки из-за прогрессирующего послеожогового рубцевания. На втором коллаже представлены фотографии 2 месяца спустя после операции рубцового выворота. Рубцовый выворот нижнего века также прогрессировал, но срочности не представлял.
Ах два. Интересный факт. Тарзорафию это рубцевание рвало дважды (фотография 1, слева сверху под свежим ожогом), варианта оттянуть экспозицию роговицы практически не оставалось.