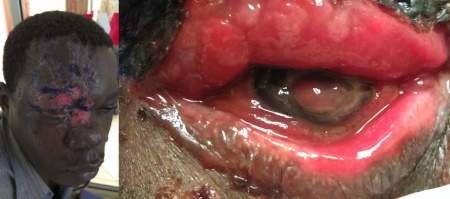
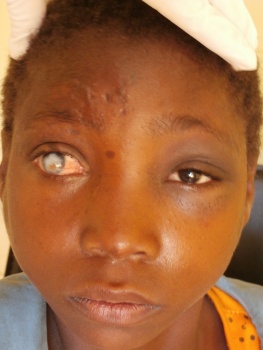
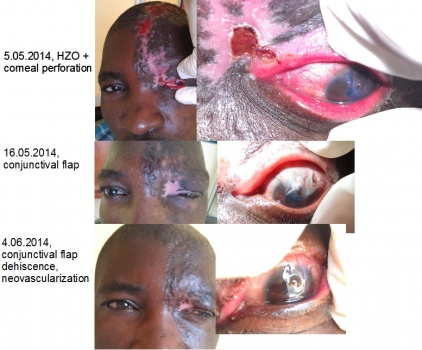
An Entity, of which I was not aware…
The role of human immunodeficiency virus in the pathogenesis of vernal keratoconjunctivitis-like disease in adults: A demographic and epidemiological study
Indian J Ophthalmol. 2020 Aug;68(8):1551-1554. doi: 10.4103/ijo.IJO_1608_19.
Authors
Anine Kritzinger 1 , Anthony G Zaborowski 1 , Wilbert Sibanda 2 , Linda Visser 1
Affiliations
1 Department of Ophthalmology, University of KwaZulu-Natal, Durban, South Africa.
2 School of Mathematics, Statistics and Computer Science, University of KwaZulu-Natal, Durban, South Africa.
PMID: 32709773
PMCID: PMC7640813
DOI: 10.4103/ijo.IJO_1608_19
Free PMC article
Abstract
Purpose: The purpose was to identify and describe patients with new-onset vernal keratoconjunctivitis-like (VKC-like) disease after puberty.
Methods: The study consisted of two parts: a prospective observational descriptive study of patients with new-onset VKC-like disease, and a case-control study to determine the relationship of a CD4 count with VKC-like disease in adults, in the setting of human immunodeficiency virus (HIV). Patients were recruited between January 2016 and November 2017 from a Provincial Eye hospital, one of two large referral hospitals in KwaZulu-Natal, South Africa. Patients presenting to the eye clinic were screened and diagnosed at the Primary Eye Care Unit. Inclusion criteria: age 15 years and older with signs and symptoms of new-onset VKC-like disease. Exclusion criteria: a history of childhood atopic diseases, atopic keratoconjunctivitis and patients who declined HIV testing. Data collected included HIV status, CD4 count, antinuclear antibodies and total serum immunoglobulin E.
Results: Thirty-three patients were included; females n = 16 and males n = 17. The mean age at presentation was 32.45 ± 9.93 years, 95% CI = 28.94-35.97. Twenty-six patients (78.8%) were HIV positive, 95% CI (62-89). The proportion of HIV positive patients was statistically different from the HIV negative group, Chi-squared = 21.866, P value <0.0001. In the group of HIV positive patients, 72% were classified as immunodeficient according to their CD4 counts. An association was proven between severely immunodeficient patients and the risk of VKC-like disease (Chi-squared = 4.992, P value = 0.0255).
Conclusion: In this cohort, a statistically significant association was found between VKC-like disease in adults and an HIV positive status. This association calls for more research on the subject.
Keywords: Allergy; VKC-like disease in adults; immunocompromised; ocular manifestations of HIV; vernal keratoconjunctivitis.