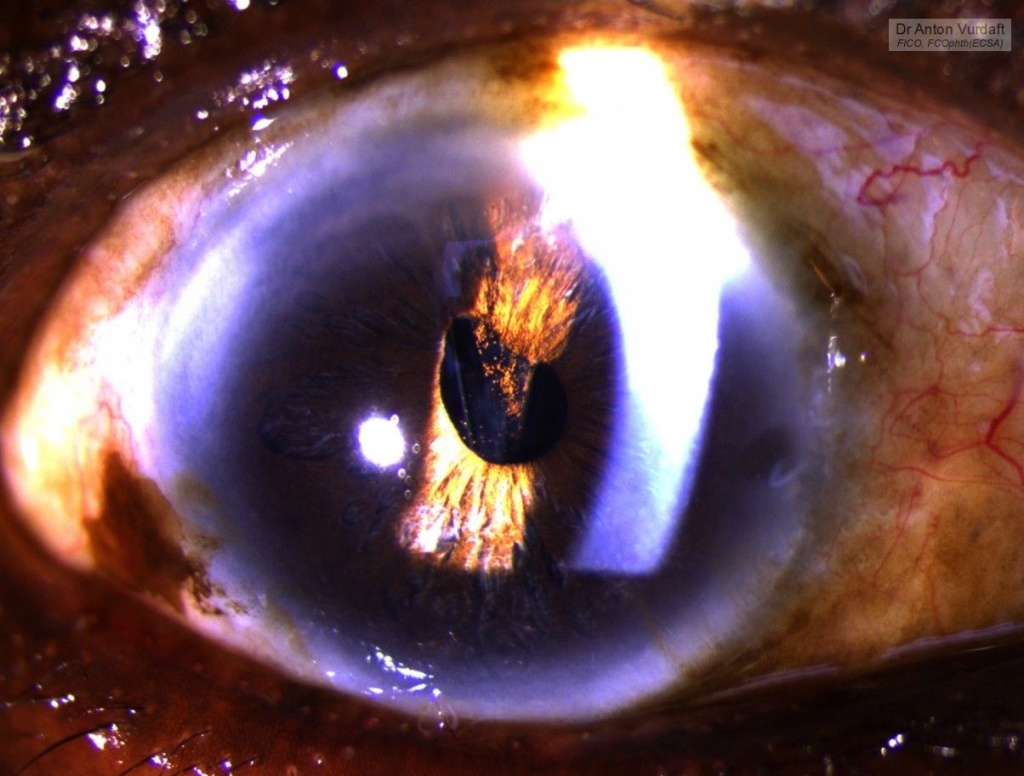
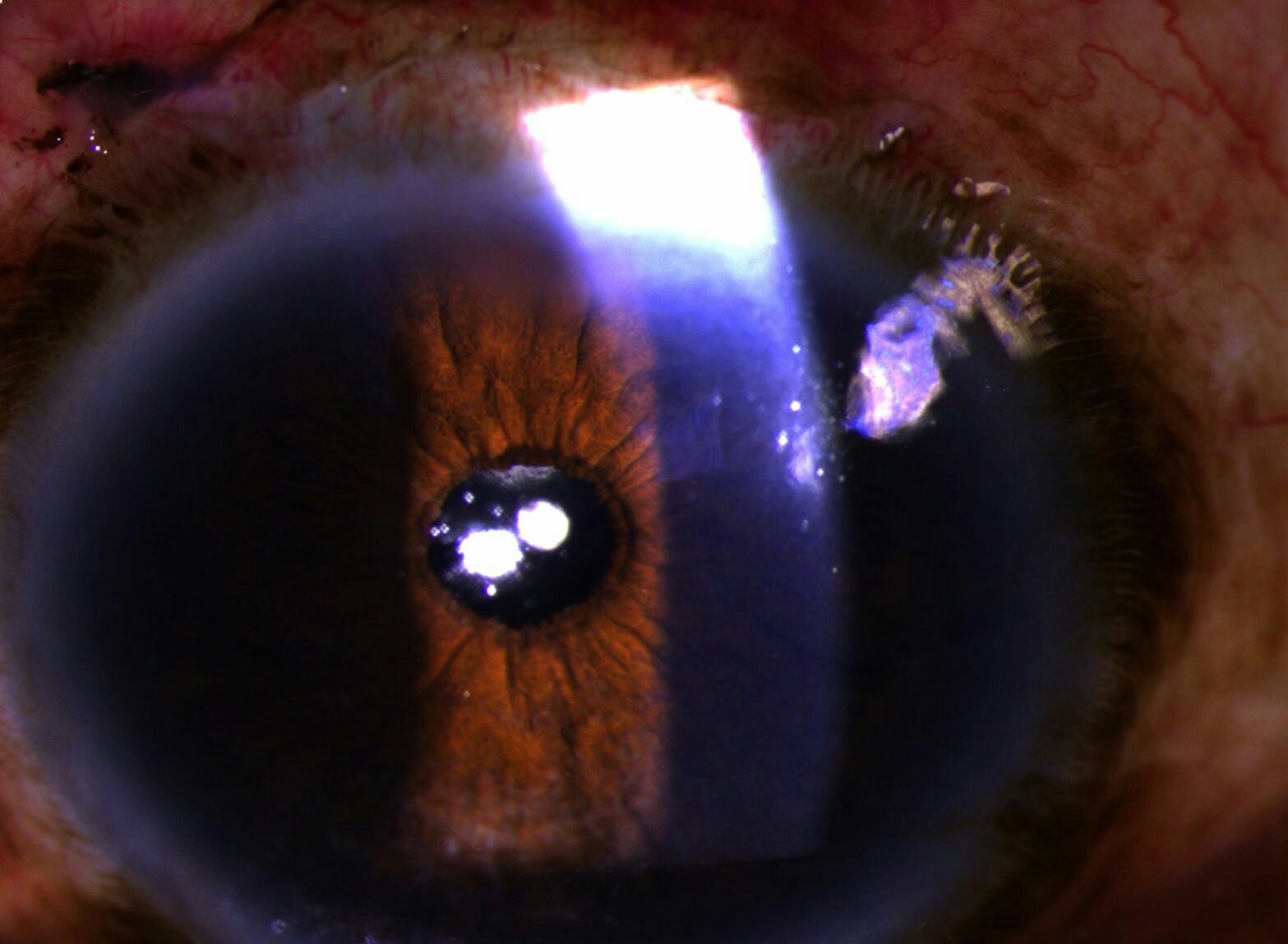
![]() EN: A case of June 2015. Classic picture of Morgagnian cataract, i.e. hypermature, white cataract, where cortex is mostly dissolved, and a rigid lens nucleus floats in the milky liquid cortical matter.
EN: A case of June 2015. Classic picture of Morgagnian cataract, i.e. hypermature, white cataract, where cortex is mostly dissolved, and a rigid lens nucleus floats in the milky liquid cortical matter.
These cases are risky because of possible secondary glaucomas (i.e., phacolytic) and because of difficulties with capsulorrhoexis. The latter requires extra caution, initial anterior capsule puncture, cortex suction and bag refill with visco.
Photos demonstrate pre-op and post-op status.
![]() RU: Случай июня 2015. Предоперационные и послеоперационные фотографии морганиевой катаракты (перезрелое твёрдое ядро купается в растворённом молочном кортексе). Опасности такой катаракты: возможная факолитическая глаукома, трудности при проведении капсулотомии или капсулорексиса.
RU: Случай июня 2015. Предоперационные и послеоперационные фотографии морганиевой катаракты (перезрелое твёрдое ядро купается в растворённом молочном кортексе). Опасности такой катаракты: возможная факолитическая глаукома, трудности при проведении капсулотомии или капсулорексиса.
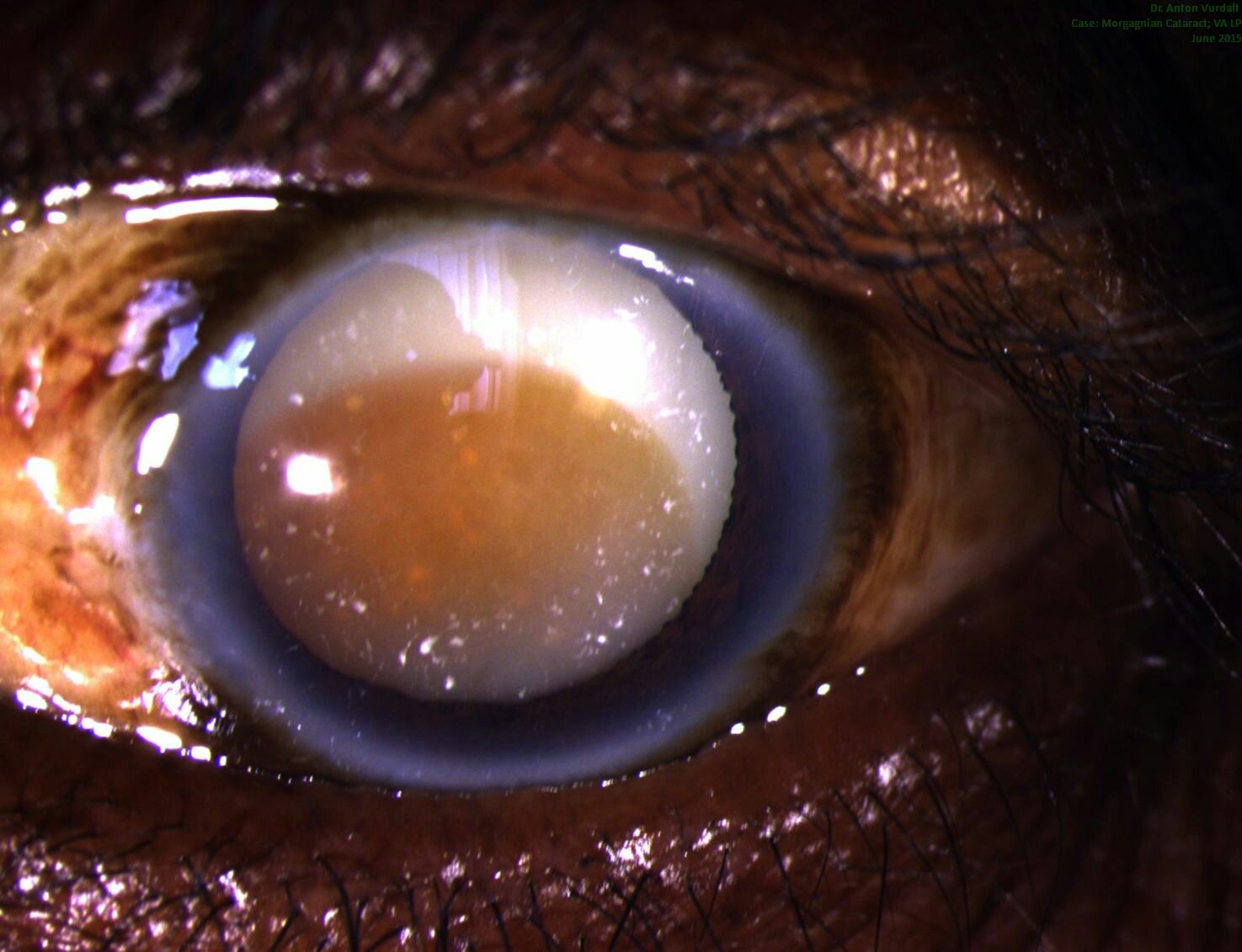
Morgagnian hypermature cataract: pre-op status
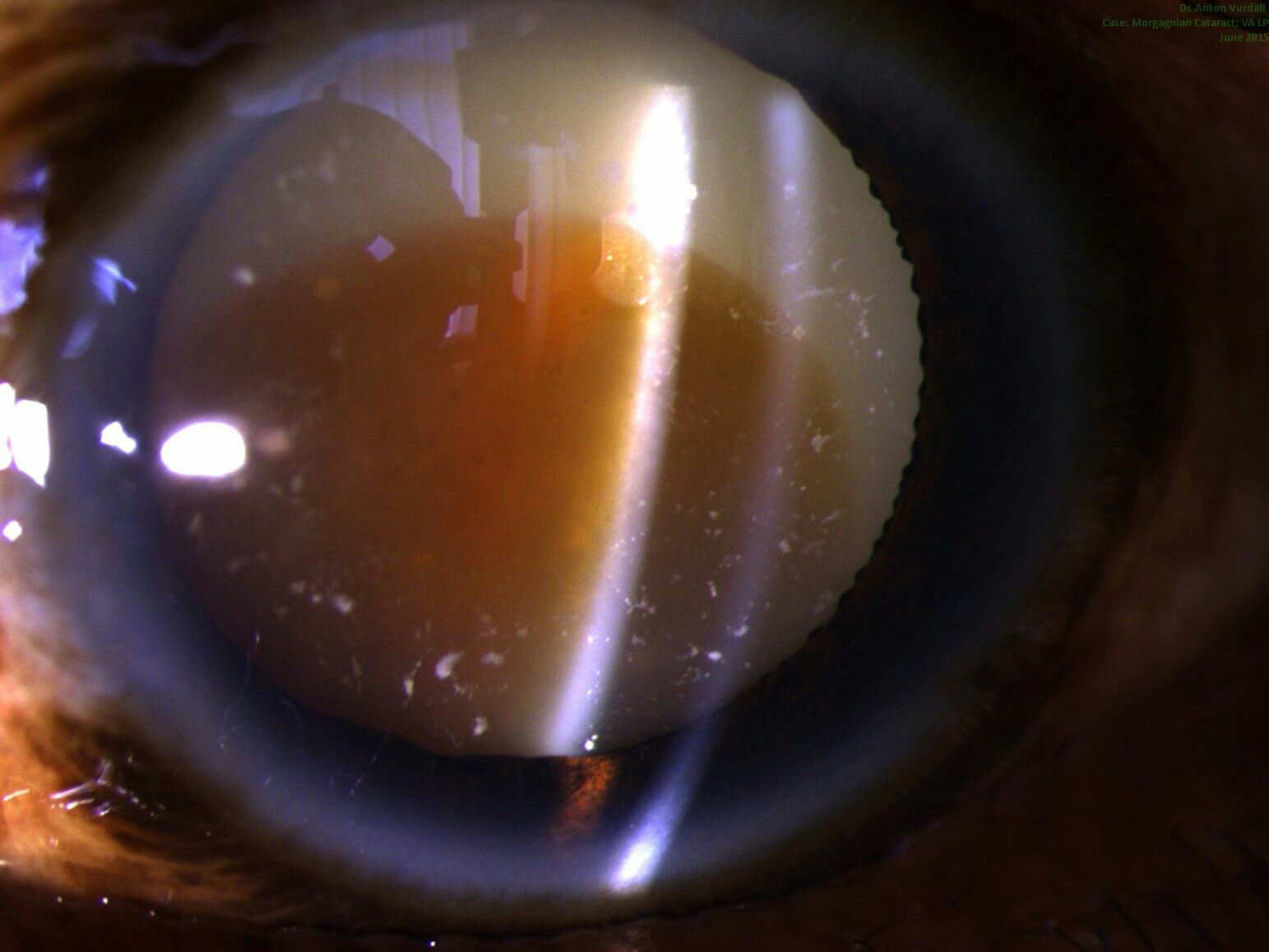
Morgagnian cataract: pre-op status
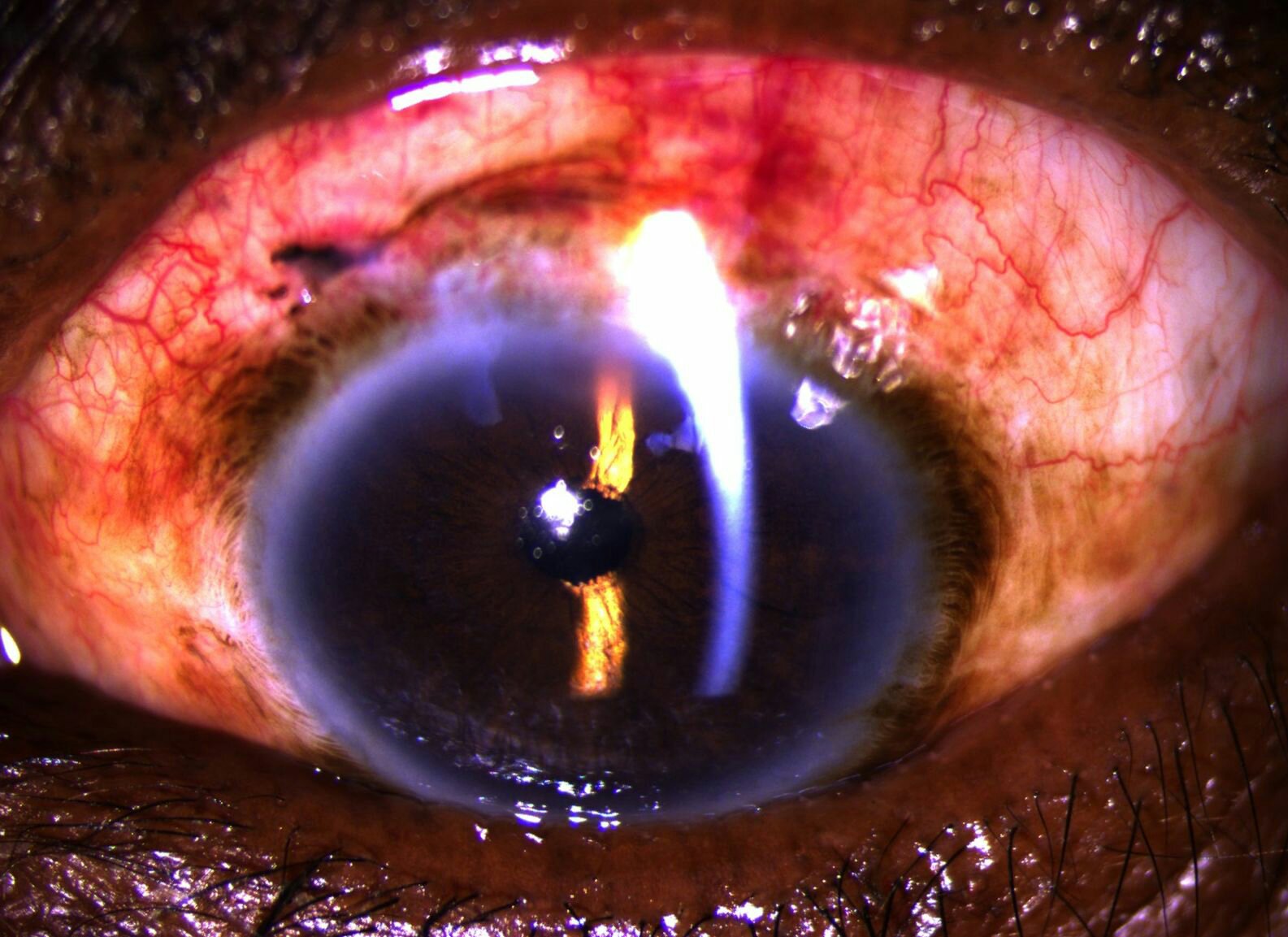
Postoperative status: SICS in Morgagnian cataract
Postoperative status: SICS in Morgagnian cataract